Changing Risk Stratification in Hypertrophic Cardiomyopathy: Extended ECG Monitoring Reveals New Insights
Core Concepts
Extended ECG monitoring in hypertrophic cardiomyopathy patients reveals significant insights into arrhythmias, impacting risk stratification and treatment decisions.
Abstract
Overview
The article discusses the importance of extended ECG monitoring in hypertrophic cardiomyopathy (HCM) patients for detecting atrial fibrillation (AFib) and nonsustained ventricular tachycardia (NSVT) to improve risk stratification and treatment decisions.
Key Highlights
Regular monitoring with a Holter monitor is crucial for HCM patients to identify AFib and NSVT.
NSVT detection influences the eligibility for an implantable cardioverter defibrillator (ICD).
Extended ECG monitoring detected significantly more clinically relevant arrhythmias compared to 24-hour monitoring.
Extended monitoring may lead to reclassification of patients into higher-risk categories for sudden cardiac death.
Extended monitoring also showed potential benefits in detecting previously undiagnosed AFib cases.
Insights
Extended ECG monitoring provides valuable data on arrhythmias, impacting treatment decisions and risk assessment.
The use of wearables for arrhythmia detection is emerging, potentially changing the landscape of monitoring practices.
The implications of increased arrhythmia detection on patient management and outcomes require further research and consideration.
Changing Risk Stratification in Hypertrophic Cardiomyopathy?
Stats
An AFib diagnosis calls for full anticoagulation due to the high risk of cerebrovascular events.
Extended ECG monitoring detected a higher incidence of clinically relevant arrhythmias compared to 24-hour monitoring (65% vs 11%, P < .001).
Extended monitoring data resulted in reclassification of patients to higher risk categories for sudden cardiac death (2.92% vs 1.74%, P < .001).
Quotes
"We are living in the era of wearables that record blood volume variations, from which heart rate and other physiologic parameters can be extracted to inform about user health."
"Extended ECG monitoring may lead to a significant increase in indications for prophylaxis with an ICD and anticoagulation, impacting patient outcomes."
Key Insights Distilled From
by Bruno Valdig... at www.medscape.com 05-16-2023
https://www.medscape.com/viewarticle/992014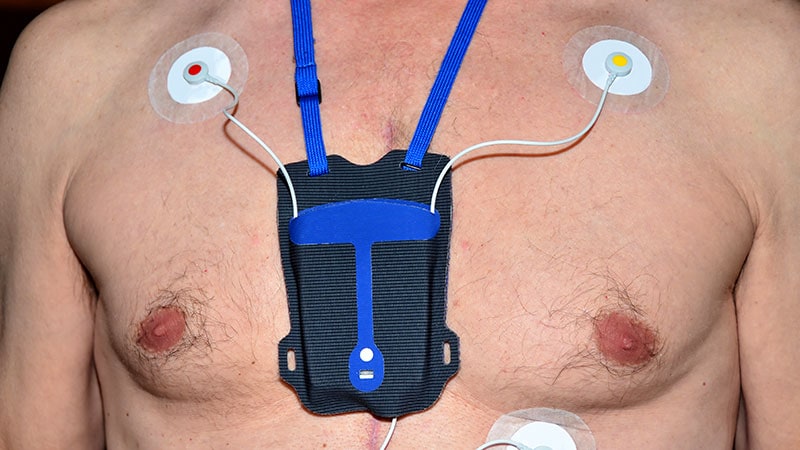
Deeper Inquiries
How can the findings from extended ECG monitoring be integrated into routine clinical practice to improve patient outcomes?
The findings from extended ECG monitoring can be integrated into routine clinical practice by establishing protocols for the systematic use of extended monitoring in patients with hypertrophic cardiomyopathy (HCM). This could involve incorporating extended monitoring as a standard part of the regular assessment for HCM patients, alongside traditional 24- or 48-hour Holter monitoring. Clinicians can use the data from extended monitoring to identify patients at higher risk of adverse events such as atrial fibrillation (AFib) or nonsustained ventricular tachycardia (NSVT) and adjust their management accordingly. Additionally, healthcare providers can develop guidelines on how to interpret the results of extended monitoring and make informed decisions regarding the need for interventions like anticoagulation or implantable cardioverter defibrillators (ICDs) based on the detected arrhythmias.
What are the potential implications of increased arrhythmia detection on healthcare resource utilization and costs?
The increased detection of arrhythmias through extended monitoring may have significant implications for healthcare resource utilization and costs. With more arrhythmias being identified, there could be a higher demand for follow-up diagnostic tests, specialist consultations, and interventions such as ICD implantation or anticoagulation therapy. This could lead to increased healthcare expenditures related to the diagnosis and management of arrhythmias in patients with HCM. Moreover, the need for additional monitoring devices and personnel to analyze the data from extended monitoring could further add to the overall costs. Healthcare systems may need to allocate resources efficiently to accommodate the increased workload resulting from the higher detection rates and ensure timely and appropriate management of patients with newly identified arrhythmias.
How can the use of wearables for arrhythmia detection be standardized and regulated to ensure patient safety and data accuracy?
Standardizing and regulating the use of wearables for arrhythmia detection is crucial to ensure patient safety and data accuracy. One approach could involve developing clear guidelines and standards for the design, validation, and clinical use of wearable devices for arrhythmia monitoring. Regulatory bodies can establish certification processes to verify the accuracy and reliability of these devices in detecting arrhythmias. Additionally, healthcare providers can implement protocols for the integration of wearable data into electronic health records, ensuring that the information is securely transmitted and easily accessible for clinical decision-making. Continuous monitoring of the performance and safety of wearables, along with regular updates to software and algorithms, can help maintain the quality and reliability of arrhythmia detection. Collaboration between healthcare professionals, device manufacturers, and regulatory agencies is essential to establish a framework that promotes the safe and effective use of wearables for arrhythmia monitoring in clinical practice.
0
