Genetic Disorder Causing Progressive Motor and Cognitive Decline in Middle-Aged Woman
The content describes the case of a 51-year-old woman presenting with worsening short-term memory, difficulty with organization and planning, and involuntary movements (chorea) in her extremities. The patient has a family history of dementia and balance problems accompanied by depression and temper outbursts.
Based on the patient's symptoms, family history, neuroimaging findings, and genetic testing, she was diagnosed with Huntington's disease (HD), an inherited, autosomal dominant, progressive, and fatal neurodegenerative disorder. HD is characterized by involuntary movements, behavioral impairment, and cognitive decline, typically affecting patients between the ages of 30 and 50.
The differential diagnosis considered other neurological conditions, including multiple sclerosis, neuroacanthocytosis, systemic lupus erythematosus, Alzheimer's disease, frontotemporal dementia, corticobasal degeneration, Parkinson's disease, and various spinocerebellar ataxias. However, the patient's presentation, family history, and genetic testing results confirmed the diagnosis of HD.
HD is caused by an expanded CAG (cytosine-adenine-guanine) repeat in the HTT gene, which codes for an abnormal version of the huntingtin protein. The number of CAG repeats determines the risk and severity of the disease, with more than 40 repeats being diagnostic for HD.
The content outlines the management of HD, which includes symptomatic treatments for chorea, behavioral and psychiatric symptoms, cognitive impairment, and seizures (in juvenile cases). Supportive care, physical and occupational therapy, and patient/family education are also crucial. Investigational therapies targeting the underlying genetic cause are being studied, but no effective treatment for preventing or reversing the progression of HD is currently available.
HD is a relentlessly progressive disorder, leading to disability and death, with a mean survival of 15-20 years from the onset of symptoms. Early diagnosis is important to provide genetic counseling, access to symptom-relieving treatments, and support for patients and their families.
Customize Summary
Rewrite with AI
Generate Citations
Translate Source
To Another Language
Generate MindMap
from source content
Visit Source
www.medscape.com
Progressive Motor, Cognitive Decline in 51-Year-Old Woman
Key Insights Distilled From
by Karen E. And... at www.medscape.com 05-01-2024
https://www.medscape.com/viewarticle/dont-miss-dx-progressive-motor-behavioral-and-cognitive-2024a10008d5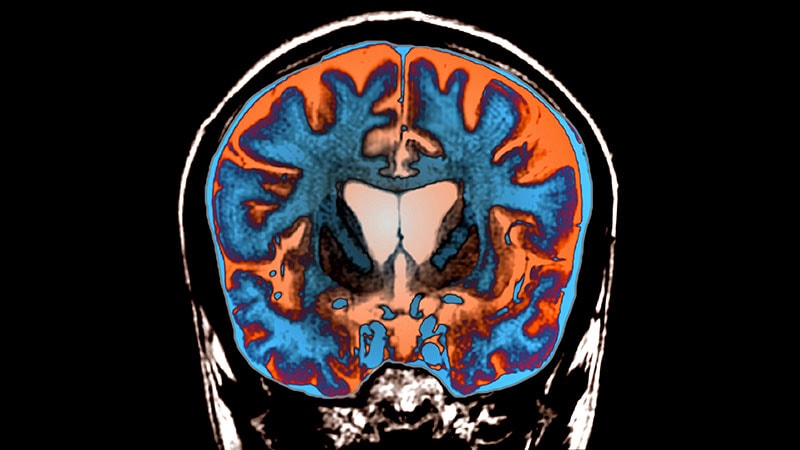
Deeper Inquiries
