Core Concepts
Andexanet alfa rapidly reduces anti-Xa activity and improves hemostatic efficacy in ICH patients on factor Xa inhibitors, despite an increased risk of thrombotic events.
Abstract
Andexanet alfa effectively reverses anticoagulation effects of factor Xa inhibitors in ICH patients.
ANNEXa-I study showed improved hemostatic efficacy with andexanet alfa but also an increased risk of thrombotic events.
Patients with ICH on factor Xa inhibitors have high hematoma expansion rates, leading to increased mortality and disability.
Trial compared andexanet alfa vs usual care in ICH patients on factor Xa inhibitors, showing superior efficacy in the andexanet group.
Andexanet alfa led to a significant reduction in anti-Xa activity and improved hemostatic efficacy compared to usual care.
Safety results indicated an increase in thrombotic events with andexanet alfa.
Further data analysis is needed to optimize patient selection and understand the balance between risks and benefits.
Andexanet Aids Hemostasis in ICH Tied to FXa Inhibitors
Stats
Andexanet alfa associated with a 92% reduction in anti-Xa activity in patients with acute major bleeding.
Good or excellent hemostatic efficacy achieved in 63.9% of patients in the andexanet arm.
Safety results showed an increase in thrombotic events in the andexanet group.
Quotes
"Andexanet can be considered for patients with ICH associated with factor Xa inhibitors but, as with many treatments, we will need to balance the benefits and risks and use careful risk stratification for patient selection." - Stuart Connolly
"While the trial clearly shows that this drug works in re-establishing effective hemostasis, this has to be balanced by the increased risk of thrombotic events." - Rustam Al-Shahi Salman
Key Insights Distilled From
by Sue Hughes at www.medscape.com 10-23-2023
https://www.medscape.com/viewarticle/997648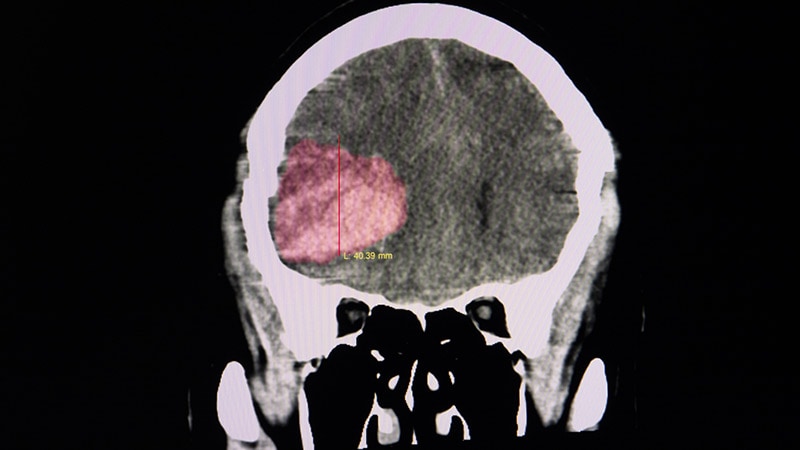
Deeper Inquiries
How can the balance between the benefits of improved hemostasis and the risks of thrombotic events be optimized in clinical practice?
In clinical practice, optimizing the balance between the benefits of improved hemostasis and the risks of thrombotic events in patients with intracerebral hemorrhage (ICH) on factor Xa inhibitors involves careful risk stratification and individualized decision-making. Physicians need to assess the patient's overall clinical status, including factors such as age, comorbidities, prior history of stroke or myocardial infarction, and the severity of the bleeding event.
To optimize this balance, it is crucial to consider the specific characteristics of each patient, such as the type and dose of factor Xa inhibitor they are on, the timing of symptom onset, and the baseline hematoma volume. Additionally, monitoring antifactor Xa levels and adjusting the dose of andexanet alfa accordingly can help tailor the treatment to each patient's needs.
Furthermore, close monitoring for signs of thrombotic events post-treatment is essential to promptly address any complications that may arise. This includes assessing for symptoms of ischemic stroke or myocardial infarction and adjusting the patient's management accordingly.
Ultimately, a multidisciplinary approach involving neurologists, hematologists, and intensivists can help optimize the balance between the benefits of improved hemostasis and the risks of thrombotic events in clinical practice.
What are the implications of the increased thrombotic events associated with andexanet alfa in ICH patients on factor Xa inhibitors?
The increased thrombotic events associated with andexanet alfa in ICH patients on factor Xa inhibitors have significant implications for clinical practice and patient management. While andexanet alfa effectively reverses the anticoagulant effects of factor Xa inhibitors and improves hemostasis in patients with ICH, the higher incidence of thrombotic events raises concerns about the overall safety of the treatment.
These implications include the need for vigilant monitoring of patients post-treatment for signs of thrombosis, such as ischemic stroke or myocardial infarction. Healthcare providers must be prepared to promptly intervene and manage these complications to prevent adverse outcomes in patients.
Additionally, the increased thrombotic events associated with andexanet alfa highlight the importance of individualized risk assessment and careful patient selection when considering the use of this reversal agent. The potential benefits of improved hemostasis must be weighed against the risks of thrombosis in each patient, taking into account their specific clinical characteristics and the urgency of the situation.
Overall, the implications of the increased thrombotic events associated with andexanet alfa underscore the need for a balanced approach to anticoagulant reversal in ICH patients, prioritizing patient safety while striving to achieve optimal outcomes.
How can the results of the ANNEXa-I trial impact the development of future treatments for ICH patients on anticoagulants?
The results of the ANNEXa-I trial can have a significant impact on the development of future treatments for ICH patients on anticoagulants by providing valuable insights into the efficacy and safety of anticoagulant reversal agents.
Firstly, the findings from the trial, which demonstrated the effectiveness of andexanet alfa in rapidly reducing antifactor Xa activity and improving hemostatic efficacy in ICH patients on factor Xa inhibitors, can inform the development of novel reversal agents with similar mechanisms of action. Researchers can use this data to design and test new agents that target specific anticoagulants and optimize hemostasis in bleeding patients.
Secondly, the observed increase in thrombotic events associated with andexanet alfa in the trial underscores the importance of evaluating the safety profile of anticoagulant reversal agents comprehensively. Future treatments must prioritize minimizing the risk of thrombosis while effectively reversing anticoagulant effects to ensure patient safety and positive clinical outcomes.
Furthermore, the ANNEXa-I trial results highlight the need for further research into the long-term clinical outcomes and cost-effectiveness of anticoagulant reversal agents in ICH patients. Future studies can build upon these findings to explore additional endpoints, such as functional outcomes and healthcare utilization, to provide a more comprehensive understanding of the benefits and risks of these treatments.
In conclusion, the results of the ANNEXa-I trial can guide the development of future treatments for ICH patients on anticoagulants by shaping the design of new reversal agents, emphasizing safety considerations, and informing future research directions in this critical area of clinical need.
0
